Radical Prostatectomy Post-Radiotherapy with Perineal Prostatic Fistula
Case description
Video case: radical prostatectomy post-radiotherapy with perineal prostatic fistula using Versius platform.
This video show an 81 year old man who underwent a robotic radical prostatectomy procedure after radiotherapy. The indication for surgery was due to a longstanding perineal prostatic fistula.
Patients undergoing radiotherapy for a prostatic adenocarcinoma Gleason 3+7 a 10 years ago, treated with total dose 68Gy.
After 5 years, evolved with infravesical obstruction and actinic cystitis.
Patient underwent prostate TURP plus 10 hyperbaric chamber sessions, even so, evolving with urinary retention and urethral stenosis.
After some urethral dilations and multiple infections, patients evolves with urinary incontinence plus urethral stenosis which allows the passage of 12Fr catheter.
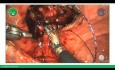
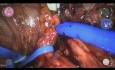
After 2 years from TURP, patient starts with repetitive inflammatory process in perineal region, with drainage of pus, as well as recurrent urinary infections. After a year with repetitive infections and three hospitalizations for sepsis, being treated only with intravenous antibiotic therapy, the patient seeks my office where I indicate parametric magnetic resonance plus pelvis with contrast that identifies a perineal prostatic fistula in evolution associated with paraprostatic collection (figure 1-3).
The indication for salvage surgery to treat the fistula as well as its possible complications was discussed with the patient and family members. The patients was stabilized with antibiotics prophylactic, and after cardiologic and anesthetic valuations, the procedure was performed.
At time of surgery until the present moment, patient presented undetectable PSA.
Patient position:
- Supine positions, with open legs, in Trendelenburg
- Use of two insufflation equipment (being expected a large amount of cauterized tissue and consequently aspiration), preventing the decrease of pneumoperitoneum pressure
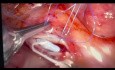
This surgery, using Versius Platform, was divided into 12 steps:
1st step: 2s.22 – Release of adhesions
2nd step: 9s.40 – Post-radiotherapy fibrosis dissection
3rd step: 1min.10s.00 – Dissection of the Santorini Plexus and Endopelvic
4th step: 2min.38s.50 – Bladder neck opening
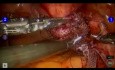
5th step: 3min.28s.73 – Identification of prostatic fistula
6th step: 3min.43s.26 – Identification of vas deferens, release of posterior and lateral planes oh the prostate. As it is not a oncological surgery, a more careful dissection was chosen, even with margins, due to the proximity to the rectum, associated with the actinic process.
7th step: 6min.37s.56 – Preservation of the apical portion of the prostate. In this moment, was impossible to access / release the urethra from post-radiotherapy fibrosis
8th step: 6min.51s.80 – Mucosal release from the prostatic ape. Preparing for future anastomosis
9th step: 7min.01s.20 – Ureteral ostium identification
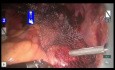
10th step: 7min.11s.82 – Bladder incision. Was not possible bring the bladder until apical prostatic position. Opted to create an incision in the bladder, remove all fibrotic tissue and rotate trhe bladder to allow a tension-free anastomosis.
11th step: 7min.35s.46 – Fibrotic bladder tissue resection
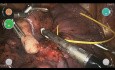
12th step: 8min.53s.21 – Closure of the posterior bladder neck “racket” with posterior bladder-prostatic (apical) anastomosis
Surgical time 240min for robotic radical prostatectomy, internal urethrotomy and perineal resection for inflammatory and infection. Patients evolve with urinary fistula, and after CT scans showing no collection, received medical discharge in the fourth postoperative day with drain and urethral catheter.
On the 9th postoperative day, the drain was removed.
On the 14th postoperative day, the urethral catheter was removed.
On the 15th postoperative day, patient presents with melena, being referred to hospital emergency. Upper digestive endoscopy shows gastric and duodenal ulcers without active bleeding. At this time, patients receive a CHAD unit. Remained two more days hospitalized.
Here it is worth mentioning that the patient was discharged home without the use of anti-inflammatory drugs after first hospitalization.
The anatomopathological exam demonstrates only fibrotic prostatic tissue.
Abstract:
I present the case of an 81-year-old male who developed a perineal prostatic fistula after 10 years of radiotherapy for the treatment of prostate cancer. Until the time of diagnosis, patient with multiple antibiotic treatments for urinary infections and purulent discharge in the perineal region. Underwent robotic radical prostatectomy using Versius platform. Due the fibrosis and “frozen” pelvis, closure of the bladder neck was performed, with anastomosis in more cranial portion of the bladder at prostatic apex. For patients without tumor recurrence, the anastomosis with prostatic apex tissue prevents a further sphincter injury, with lower tension anastomosis and easier confection.
Robotic-assisted laparoscopic prostatectomy
Sharma NL, Shah NC, Neal DE.Br J Cancer. 2009 Nov 3;101(9):1491-6. doi: 10.1038/sj.bjc.6605341. Epub 2009 Sep 29.PMID: 19861995 Free PMC article. Review.
Historical Considerations and Surgical Quality Improvement in Robotic Prostatectomy.
Omil-Lima DO, Gupta K, Calaway AC, Zell MA.Urol Clin North Am. 2021 Feb;48(1):35-44. doi: 10.1016/j.ucl.2020.09.015.PMID: 33218592 Review.
Vesicocutaneous fistula presenting 17 years post-radiotherapy for prostate cancer.
Vadhwana B, Batura D.Int Urol Nephrol. 2015 Apr;47(4):645-6. doi: 10.1007/s11255-015-0941-0. Epub 2015 Mar 11.PMID: 25758012 No abstract available.
Robotic Salvage Seminal Vesiculectomy for radio-recurrent prostate cancer post LDR brachytherapy following multiple negative trans-perineal biopsies.
Katelaris DA, Gibson DD, Nalavenkata DS, Thompson DJ.Urol Case Rep. 2022 Mar 25;43:102064. doi: 10.1016/j.eucr.2022.102064. eCollection 2022 Jul.PMID: 35368980