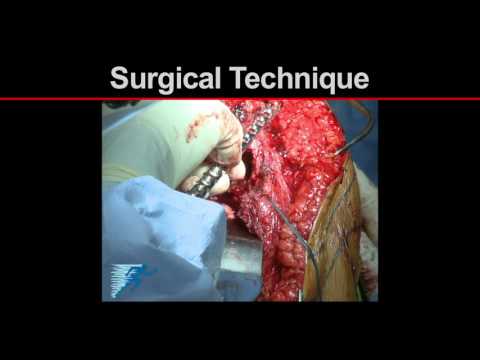
Athletic Field Assessment | Shoulder Evaluation | Shoulder Dislocation
Case description
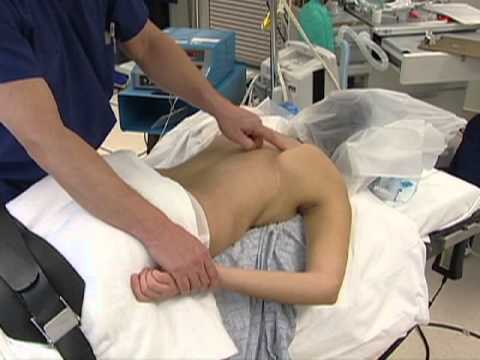
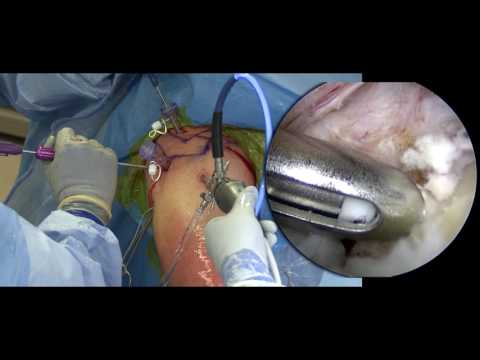
In this athlete has been injured and has gotten into a training facility on a stretcher, you can also do this on the field. If they have pads on or protective equipment, you will need to remove those, or examine the patient with the pads on. The first thing to do is ask the patient where it hurts. In this case, there is some deformity of the shoulder and has a true glenohumeral dislocation - there will be fullness in the anterior part of the shoulder. If there is a posterior dislocation, you may see some hallowing our and the coracoid may be more prominent. If there is a clavicle fracture, you will see some deformity up along the clavicle. Generally, if they have a dislocation they will hold their arm in a protective position.
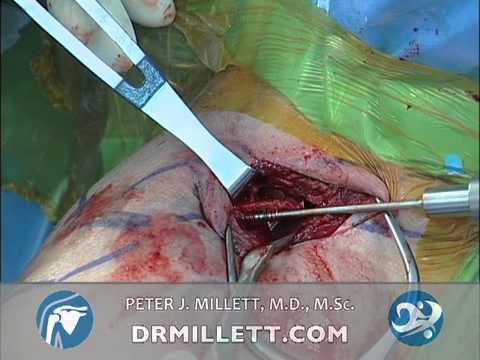
The next step is to palpate the shoulder. It is generally best to palpate areas that do not hurt and then move to more tender spots. You can start on the forearm, humerus, clavicle, and scapula. You may want to assess motion during this time.
The next step, you have determined that the patient has a shoulder dislocation, you assess their neurovascular status and their motor function in their arm. You can feel the radial pulse, good capillary refill in their fingers, then it is unlikely that there is a vascular injury. The next step would be to to a motor assessment. You can ask them to move their fingers and wrist. You can support the humerus and ask them to flex and extend their elbow. The patient can usually do that with a shoulder dislocation. The last thing we will check is the sensory function. The most commonly injured nerve is the axillary nerve. It is very rare that it is completely severed. The best way to assess that is to assess the sensory area just lateral to the elbow.
The final step would be to assess the range of motion. You have determined that the neurovascular status is intact. The crepitation is intact. Generally, Dr. Millett does a gentile external rotation and they frequently have significant guarding, but if you can get them to relax the shoulder will reduce spontaneously. Many times, they will not allow you to externally rotate.
If a patient has a posterior dislocation, they will not be able to rotate beyond neutral, because their humeral head will be impinging on the glenoid, so that loss of motion can be indicative of a posterior shoulder dislocation.
Final word, many of these athletes are contact athletes, which means they will have equipment on. The question comes on if you should remove the equipment before you assess them or after you assess them. I think it is simple to do these assessments with these pads on. If the shoulder does not reduce, you will generally have to take the pads off in order to do a manipulative reduction. Sometimes the shoulder will reduce when taking the pads off.